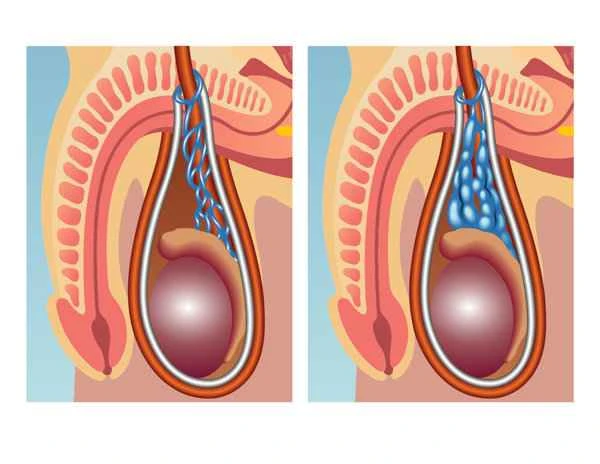
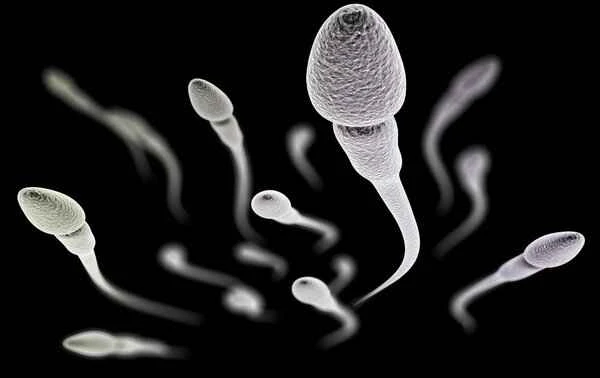
The diagnosis of congenital asthenospermia mainly relies on the results of semen analysis.

Determining congenital asthenospermia requires semen analysis, which is fundamental for assessing male fertility. Semen analysis includes testing semen volume, sperm concentration, sperm motility, and sperm morphology. Congenital asthenospermia is typically characterized by a significantly lower sperm count than the normal range, generally defined as a sperm concentration below 15 million/ml or a total sperm count below 39 million. A detailed medical history and physical examination are also necessary to rule out acquired factors causing asthenospermia, such as infection, hormonal abnormalities, and lifestyle habits. If these acquired factors are ruled out, and the semen analysis results remain abnormal, the possibility of congenital asthenospermia can be considered.

In addition to semen analysis, doctors may recommend genetic testing, such as chromosome analysis or gene testing, to further confirm whether there are genetic factors causing spermatogenesis disorders. Blood tests can also help identify any abnormal hormone levels, such as low testosterone levels, which can affect sperm production and quality. By combining the results of these tests, doctors can more accurately determine whether it is congenital asthenospermia and develop appropriate treatment and management plans.
[Management Tip:]
1. Perform semen analysis regularly to monitor sperm count and quality.
2. Avoid high-temperature environments to reduce heat damage to the testicles.
3. Maintain healthy lifestyle habits, including a balanced diet and moderate exercise.
4. If persistent infertility symptoms occur, seek medical advice promptly.